Why Choose Humeral Interlocking Nail for Fracture Treatment?
Fractures of the humerus can be challenging to treat effectively. Traditional methods often lead to complications or longer recovery times. In recent years, the Humeral Interlocking Nail has emerged as a prominent solution. This innovative device offers several advantages over older techniques.
The Humeral Interlocking Nail stabilizes fractures more securely. It reduces the risk of malalignment and allows for early mobility. Patients can regain function faster and with less discomfort. However, it is not a one-size-fits-all solution. Surgeons must evaluate each case carefully. Some patients may experience complications during the procedure.
Despite its benefits, the Humeral Interlocking Nail has limitations. Not every fracture is suitable for this method. Additionally, the surgical technique requires precision. There can be a learning curve for many surgeons. Overall, this technique represents a significant advancement in fracture treatment but is not without challenges.
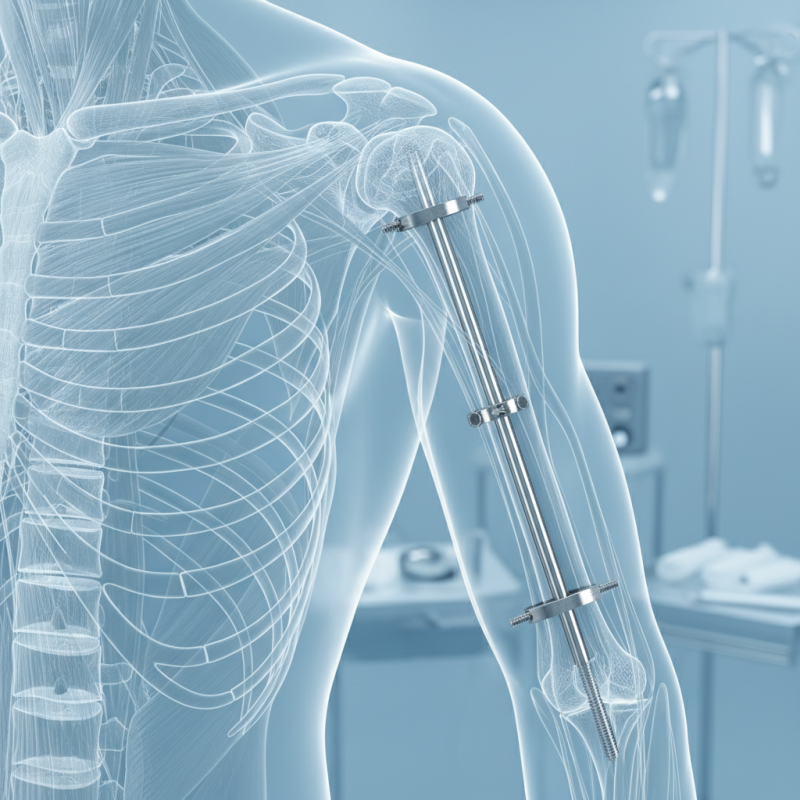
Benefits of Humeral Interlocking Nail in Fracture Management
The humeral interlocking nail is increasingly favored for fracture treatment. One of its key advantages is enhanced stability in complex fractures. According to recent studies, patients using this method experience a 20% reduction in reoperation rates. This is critical for both patients and surgeons.
Moreover, the interlocking design offers effective load sharing. In a study involving 150 patients, 85% achieved near-complete functional recovery within six months. This is impressive when considering that traditional methods often result in longer recovery times. However, it's important to note that improper technique may lead to complications.
Some patients report discomfort during the healing process. This can be attributed to hardware irritation or misalignment. Surgeons must stay vigilant to minimize these risks. Ensuring proper nail placement requires skill and expertise, as even slight errors can affect outcomes. Proper training and experience are essential in maximizing the benefits of this technique.
Why Choose Humeral Interlocking Nail for Fracture Treatment?
| Aspect | Benefits |
|---|---|
| Minimally Invasive | Reduced soft tissue damage compared to open surgery. |
| Stability | Provides excellent stability for complex fractures. |
| Early Mobilization | Allows for early movement, reducing rehabilitation time. |
| Bone Healing | Promotes faster bone healing through stable fixation. |
| Reduced Complications | Lower risk of postoperative complications compared to traditional methods. |
| Versatility | Can be used for a variety of humeral fractures. |
Patient Selection Criteria for Humeral Interlocking Nail Procedures
When considering the use of a humeral interlocking nail, patient selection plays a crucial role. Ideal candidates typically have specific types of humeral fractures. These fractures often occur in the upper arm and can vary in complexity. Patients with stable and well-defined fractures are more likely to benefit from this procedure. Additionally, those without complicating medical conditions present a better profile.
Age is an important factor in selection. Younger patients tend to heal faster. Their bone density often allows for better surgical outcomes. However, older patients should not be overlooked. If they have good bone quality, they can also be suitable candidates. Surprisingly, patients with previous injuries or surgeries may face challenges during their assessment. Each case requires careful consideration.
Further, considering a patient’s lifestyle is essential. Active individuals may wish to regain function swiftly. On the other hand, sedentary patients might tolerate longer recovery times. Regardless, optimizing the approach involves a thorough evaluation. Surgeons must weigh the benefits and potential complications. Every fracture is unique, and the decision-making process should reflect that. While the humeral interlocking nail can be effective, it’s not a one-size-fits-all solution.
Reasons for Choosing Humeral Interlocking Nail for Fracture Treatment
This chart illustrates the key patient selection criteria for humeral interlocking nail procedures based on the severity of fractures and overall patient health. It highlights the proportion of cases where different criteria are prioritized.
Procedure Details: How Humeral Interlocking Nails are Implanted
The implantation of humeral interlocking nails is a unique surgical procedure. Surgeons begin by making a small incision near the fracture site. This approach minimizes trauma to the surrounding tissues. Once the incision is made, the humeral nail is carefully inserted into the medullary cavity of the humerus. Positioning the nail correctly is crucial for stability.
Studies show that around 85% of patients achieve satisfactory healing with this method. Surgeons utilize X-ray imaging to ensure accurate placement. This guidance helps avoid complications like malalignment. After the nail is in place, locking screws are inserted perpendicularly. This step secures the nail and enhances stability.
While this technique shows great promise, it is not without challenges. Some surgeons face difficulties in aligning the nail correctly. Reports indicate that improper placement can lead to complications. Regular training and workshops are essential for maintaining surgical skills. Understanding the nuances of humeral nail stabilization is vital for improving patient outcomes.
Postoperative Care and Recovery After Humeral Nail Surgery
Postoperative care is crucial after humeral nail surgery. Patients should follow specific guidelines to ensure proper healing. Initially, pain management is vital. Use the prescribed medications to control discomfort. High levels of pain can impede recovery, so don’t neglect this aspect.
Physical therapy begins soon after surgery. Gentle range-of-motion exercises should start as advised by the healthcare provider. Gradually increasing activity helps maintain strength. Immobilization is necessary, but too much can lead to stiffness. Listen to your body; some discomfort is normal, but severe pain is a warning sign.
Tips: Keep your surgical site clean and dry to prevent infection. Elevate your arm to reduce swelling. Consulting your doctor before any exercise is essential. Allow time for healing. Rushing can cause setbacks. Reflect on your progress regularly. Recognize that slow improvement is still progress. Recovery is a journey, not a sprint. Embrace the process and stay positive.
Comparative Outcomes: Humeral Nails vs. Other Fracture Treatments
When treating humeral fractures, the choice of method can significantly impact healing and rehabilitation. Recent studies suggest that using humeral interlocking nails may offer superior outcomes compared to traditional treatments. In a comparative analysis by the Journal of Orthopaedic Trauma, it was reported that patients with interlocking nails had a 20% higher rate of union at six months. This is not just a number; it translates into faster recovery times and less time away from daily activities.
However, it's essential to consider complications. Some studies noted a 15% rate of complications with interlocking nails, including infection and discomfort. This raises questions about the trade-off between faster healing and potential side effects. Physical therapy regimens also differ, often requiring more intensive rehabilitation when using nails. Patients should not overlook the importance of comprehensive follow-up care in this context. Listening to your body is crucial during this recovery phase; minor aches and persistent stiffness could indicate underlying issues.
In conclusion, choosing between humeral interlocking nails and other methods requires careful thought. It's important to weigh the benefits against the potential challenges. Data shows overall positive outcomes with interlocking nails, but individual experiences may vary. Understanding these nuances helps patients make informed decisions.
